Osteoporosis is a bone disease that causes our bones to become weak and more likely to a fracture in a longer duration of time. It is also known as a “silent disease” because the bones become brittle without any symptoms. Fractures can happen in any bone, but osteoporosis-related fractures mostly occur in the spine, hip, and wrist. A bone is a living tissue that keeps on changing through a process called remodeling – older bones making way to build new bones. When people reach their 40s, the peak of their bone density slowly starts to decrease. At this age in life, it becomes crucial to know the importance of bone health.
Bone is living tissue. To keep bones strong, your body breaks down old bone and replaces it with new bone tissue. Sometime around age 30, bone mass stops increasing, and the goal for bone health is to keep as much bone as possible for as long as you can. As people enter their 40s and 50s, more bone may be broken down than is replaced.
A close look at the inside of bone shows something like a honeycomb. When you have osteoporosis, the spaces in this honeycomb grow larger, and the bone that forms the honeycomb gets smaller. The outer shell of your bones also gets thinner. All of this makes your bones weaker.
Bone loss before osteoporosis (osteopenia)
The stage before osteoporosis is called osteopenia. This is when a bone density scan shows you have lower bone density than the average for your age, but not low enough to be classed as osteoporosis.
Osteopenia does not always lead to osteoporosis. It depends on many factors.
If you have osteopenia, there are steps you can take to keep your bones healthy and reduce your risk of developing osteoporosis.
Your doctor may also prescribe one of the bone-strengthening treatments that are given to people with osteoporosis, depending on how weak your bones are and your risk of breaking a bone.
Symptoms
During the early stages of bone loss, there are typically no symptoms. The first symptom of osteoporosis is the fracture or breaking of bone because of a minor fall. Some of the other symptoms include:
- Stress fractures (or tiny cracks in a bone) that feel like joint or muscle pain
- Gradual height loss
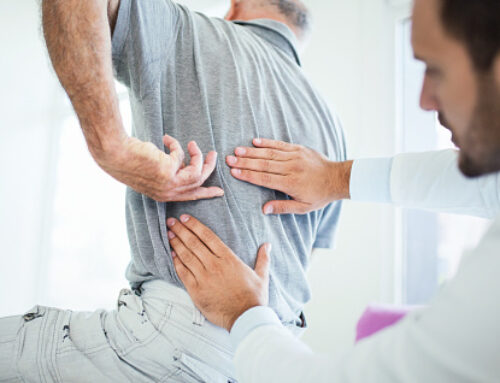
- Back pain
- Shortness of breath (due to compressed disks)
- Change in posture
Who has osteoporosis?
Although osteoporosis can strike at any age, it is most common among older people, especially older women. Men also have this disease. White and Asian women are most likely to have osteoporosis. Other women at great risk include those who:
- Have a family history of broken bones or osteoporosis
- Have broken a bone after age 50
- Had surgery to remove their ovaries before their periods stopped
- Had early menopause
- Have not gotten enough calcium and/or vitamin D throughout their lives
- Had extended bed rest or were physically inactive
- Smoke (smokers may absorb less calcium from their diets)
- Take certain medications, including medicines for arthritis and asthma and some cancer drugs
- Used certain medicines for a long time
- Have a small body frame
The risk of osteoporosis grows as you get older. At the time of menopause, women may lose bone quickly for several years. After that, the loss slows down but continues. In men, the loss of bone mass is slower. But, by age 65 or 70, men and women are losing bone at the same rate.
Risk factors
Certain factors raises your risk of getting osteoporosis:
- Age – With age, our bones naturally become thinner and this increases the risk of getting osteoporosis
- Your sex – Being a woman raises your risk of developing osteoporosis
- Race – Caucasian and Asian women are at a higher risk
- Body weight – Thin people are at higher risk of developing osteoporosis
- Family history – If one of your parents has had a broken bone, especially a broken hip, you are at greater risk of developing osteoporosis
- Excessive alcohol consumption and smoking
- Dietary factors – It is more likely in people with low calcium and vitamin D intake
- Steroids and other medications – Oral or injected corticosteroid medications may hinder the bone-rebuilding process
- Medical conditions – Celiac disease, inflammatory bowel disease, kidney or liver diseases, cancer, and rheumatoid arthritis, can raise the risk of developing the disease
- Sedentary lifestyle – People who spend a lot of time sitting at a desk are more prone to osteoporosis
What is osteopenia?
Whether your doctor calls it osteopenia or low bone mass, consider it a warning. Bone loss has started, but you can still take action to keep your bones strong and maybe prevent osteoporosis later in life. That way you will be less likely to break a wrist, hip, or vertebrae (bone in your spine) when you are older.
Can my bones be tested?
For some people, the first sign of osteoporosis is to realize they are getting shorter or to break a bone easily. Don’t wait until that happens to see if you have osteoporosis. You can have a bone density test to find out how strong your bones are.
The U.S. Preventive Services Task Force recommends that women aged 65 and older be screened (tested) for osteoporosis, as well as women under age 65 who are at increased risk for an osteoporosis-related fracture.
A bone mineral density test compares your bone density to the bones of an average healthy young adult. The test result, known as a T-score, tells you how strong your bones are, whether you have osteoporosis or osteopenia, and your risk for having a fracture.
Complications
- Pain – The disease weakens the bones which results in hunched posture, loss of height, and back pain
- Limited mobility – Fractures can cause limited mobility or the inability to stand up for a long period. Being physically inactive can cause you to gain weight and increase the stress on bones
- Nursing home care – People who have a hip fracture may require long-term nursing care. A bed-ridden person is more likely to experience cardiovascular complications and increased susceptibility to infectious diseases
Diagnosis of osteoporosis
If your doctor suspects a case of osteoporosis, you may be required to take a bone mineral density (BMD) test.
DEXA Scan
BMD tests are also called dual-energy X-ray absorptiometry (DEXA or DXA). The amount of radiation used in these scans is very small as it helps find out how solid the bones of the hip, wrist, and spine are. DEXA is a simple, quick, and non-invasive test, that is usually performed on the lower spine and hips. The scan helps evaluate the risk of osteoporosis fractures and monitor a person’s response to treatment.
The results of a DEXA scan is measured in form of T scores or Z scores. While the T scores compare bone density with that of a healthy 30-year-old of the same sex, the Z scores compare bone density to a similar population as the patient in terms of age, size, and sex.
Blood tests
A blood test can help find out:
Vitamin D deficiency
Calcium levels or deficiency
Hormone levels
Medical conditions including parathyroid and thyroid malfunctioning can cause bone loss. Testing for thyroid function and testosterone levels in men can help find out the cause of osteoporosis.
Other tests
Your doctor can also order an ultrasound scan of the heel bone to assess osteoporosis.
How can I keep my bones strong? Preventing osteoporosis
There are things you should do at any age to prevent weakened bones. Eating foods that are rich in calcium and vitamin D is important. So is regular weight-bearing exercise, such as weight training, walking, hiking, jogging, climbing stairs, tennis, and dancing.
If you have osteoporosis, avoid activities that involve twisting your spine or bending forward from the waist, such as conventional sit-ups, toe touches, or swinging a golf club.
What medications are used to treat osteoporosis?
There are several classes of medications used to treat osteoporosis. Your healthcare provider will work with you to find the best fit. It’s not really possible to say there is one best medication to treat osteoporosis. The ‘best’ treatment is the one that is best for you.
Hormone and hormone-related therapy
This class includes estrogen, testosterone and the selective estrogen receptor modulator raloxifene (Evista®). Because of the potential for blood clots, certain cancers and heart disease, estrogen therapy is likely to be used in women who need to treat menopause symptoms and in younger women.
Testosterone might be prescribed to increase your bone density if you are a man with low levels of this hormone.
Raloxifene acts like estrogen with the bones. The drug is available in tablet form and is taken every day. In addition to treating osteoporosis, raloxifene might be used to reduce the risk of breast cancer in some women. For osteoporosis, raloxifene is generally used for five years.
Calcitonin-salmon (Fortical® and Miacalcin®) is a synthetic hormone. It reduces the chance of spine fractures, but not necessarily hip fractures or other types of breaks. It can be injected or it can be inhaled through the nose. Side effects include runny nose or nosebleed and headaches for the inhaled form. Side effects include rashes and flushing for the injected form. It is not recommended as a first choice. There are possible more serious side effects, including a weak link to cancer.
Bisphosphonates
Bisphosphonate osteoporosis treatments are considered antiresorptive drugs. They stop the body from re-absorbing bone tissue. There are several formulations with various dosing schemes (monthly, daily, weekly and even yearly) and different brands:
- Alendronate: Fosamax®, Fosamax Plus D®, Binosto®.
- Ibandronate: Boniva®.
- Risedronate: Actonel®, Atelvia®.
- Zoledronic acid: Reclast®.
You may be able to stop taking bisphosphonates after three to five years and still get benefits after you stop. Also, these drugs are available as generic drugs. Of these products, Boniva and Atelvia are recommended only for women, while the others can be used by both women and men.
Possible side effects of bisphosphonates include flu-like symptoms (fever, headache), heartburn, and impaired kidney function. There are potentially serious side effects also, such as the rare occurrence of jaw bone damage (osteonecrosis of the jaw) or atypical femur fractures (low trauma fractures of the thigh). The risk of these rare events increases with prolonged use of the medication (>5 years).
Biologics
Denosumab (Prolia®) is product that is available as an injection given every six months to women and men. It is often used when other treatments have failed. Denosumab can be used even in some cases of reduced kidney function. Its long-term effects are not yet known, but there are potentially serious side effects. These include possible problems with bones in the thigh or jaw and serious infection.
Anabolic agents
These products build bone in people who have osteoporosis. There are three of these products currently approved:
- Romososumab-aqqg (Evenity®) has been approved for postmenopausal women who are at a high risk of fracture. The product both enables new bone formation and decreases the breakdown of bone. You will get two injections, one right after the other, once per month. The time limit is one year of these injections.
- Teriparatide (Forteo®) and Abaloparatide (Tymlos®) are injectable drugs given daily for 2 years. They are parathyroid hormones, or products similar in many ways to the hormones.
When should osteoporosis be treated with medication?
Women whose bone density test shows T-scores of -2.5 or lower, such as -3.3 or -3.8, should begin therapy to reduce their risk of fracture. Many women need treatment if they have osteopenia, which is bone weakness that is not as severe as osteoporosis. Your doctor might use the World Health Organization fracture risk assessment tool, or FRAX, to see if you qualify for treatment based on your risk factors and bone density results. People who have had a typical osteoporosis fracture, such as that of the wrist, spine or hip, should also be treated (sometimes even if the bone density results are normal).
Supplements
It’s important to remember that dietary supplements, although available everywhere over-the-counter and online, aren’t regulated in the same way that prescription medications are. Also, even though something is ‘natural,’ that doesn’t mean that it is safe for everyone at all times.
You might be told by your healthcare provider to get adequate amounts of calcium and vitamin D. This is important if you have osteoporosis or if you are trying to prevent it. It’s best if you can meet those needs with a food plan, but you might not be able to do that. There are plant-based calcium supplements, some of which are based on algae.
The recommended amount of daily calcium intake is 1,000 mg to 1,200 mg daily via diet and/or supplements. Taking more than this amount of calcium has not been shown to provide additional bone strength but may be associated with an increased risk of kidney stones, calcium buildup in the blood vessels and constipation.
There are different ideas about the necessary levels of vitamin D, but it’s true that many people do not have adequate levels and might need to take supplements. Your healthcare provider might test your blood levels and then make recommendations based on these results.
There are other supplements that have been touted as useful for osteoporosis. One of these is strontium, which has never been approved in the U.S. for osteoporosis. A prescription version of strontium ranelate had been available in the E.U., but it was taken off the market due to serious side effects.
You and your healthcare provider will always need to discuss whether the benefits of taking something, whether is a prescription drug or a supplement, outweigh the risks.
What can I do for my osteoporosis?
Treating osteoporosis means stopping the bone loss and rebuilding bone to prevent breaks. Healthy lifestyle choices such as proper diet, exercise, and medications can help prevent further bone loss and reduce the risk of fractures.
But, lifestyle changes may not be enough if you have lost a lot of bone density. There are also several medicines to think about. Some will slow your bone loss, and others can help rebuild bone. Talk with your doctor to see if medicines might work to treat your osteoporosis.
Can I avoid falling?
When your bones are weak, a simple fall can cause a broken bone. This can mean a trip to the hospital and maybe surgery. It might also mean being laid up for a long time, especially in the case of a hip fracture. So, it is important to prevent falls.
How can you prevent osteoporosis?
Your diet and lifestyle are two important risk factors you can control to prevent osteoporosis. Replacing lost estrogen with hormone therapy also provides a strong defense against osteoporosis in postmenopausal women.
Diet
To maintain strong, healthy bones, you need a diet rich in calcium throughout your life. One cup of skim or 1 percent fat milk contains 300 milligrams of calcium.
Besides dairy products, other good sources of calcium are salmon with bones, sardines, kale, broccoli, calcium-fortified juices and breads, dried figs, and calcium supplements. It is best to try to get the calcium from food and drink.
For those who need supplements, remember that the body can only absorb 500 mg of calcium at a time. You should take your calcium supplements in divided doses, since anything more than 500 mg will not be absorbed.
Recommended daily allowance of calcium
| Age and sex | Amount |
|---|---|
| Adults, 19-50 years | 1,000 mg |
| Adult men, 51-70 years | 1,000 mg |
| Adult women, 51-70 years | 1,200 mg |
| Adults, 71 years old and older | 1,200 mg |
| Pregnant and breastfeeding teens | 1,300 mg |
| Pregnant and breastfeeding adults | 1,000 mg |
Vitamin D is also important because it enables the body to absorb calcium. The recommended daily allowances of vitamin D are listed below. Vitamin D can also be obtained from sunlight exposure a few times a week or by drinking fortified milk.
Recommended daily allowance of Vitamin D
| People by age | Amount |
|---|---|
| Infants 0-6 Months | 400 IU |
| Infants 6-12 months | 400 IU |
| 1-3 years old | 600 IU |
| 4-8 years old | 600 IU |
| 9-70 years old | 800 IU |
| Over 70 years old | 800 IU |
| 14-50 years old, pregnant/lactating | 600 IU |
Talk with your healthcare provider about these numbers. In some cases, you might be told to take more vitamin D. Your provider might also have suggestions about the calcium type; for instance, you might be told to take calcium citrate instead of calcium carbonate. Calcium citrate does not need acid to work, so it may be a better choice for people who take antacids.
Lifestyle
Maintaining a healthy lifestyle can reduce the degree of bone loss. Begin a regular exercise program. Exercises that make your muscles work against gravity (such as walking, jogging, aerobics, and weightlifting) are best for strengthening bones.
Do not drink too much alcohol. Do not have excessive amounts of caffeine. Don’t use tobacco at all.
Do men have osteoporosis?
Osteoporosis is not just a woman’s disease. Not as many men have it as women do, maybe because most men start with more bone density. As they age, men lose bone density more slowly than women. But, men need to be aware of osteoporosis.
Experts don’t know as much about this disease in men as they do in women. However, many of the things that put men at risk are the same as those for women, including family history, not enough calcium or vitamin D, and too little exercise. Low levels of testosterone, too much alcohol, taking certain drugs, and smoking are other risk factors.
Older men who break a bone easily or are at risk for osteoporosis should talk with their doctors about testing and treatment.
Living with osteoporosis
If you’re diagnosed with osteoporosis, there are steps you can take to reduce your chances of a fall, such as removing hazards from your home and having regular sight tests and hearing tests.
To help you recover from a fracture, you can try using:
- hot and cold treatments such as warm baths and cold packs
- transcutaneous electrical nerve stimulation (TENS) – where a small battery-operated device is used to stimulate the nerves and reduce pain
- relaxation techniques
Speak to your GP or nurse if you’re worried about living with a long-term condition. They may be able to answer any questions you have.
You may also find it helpful to talk to a trained counsellor or psychologist, or other people with the condition.